 An international team led by researchers at Colorado State University has found that human contact with wild armadillos — including eating the meat — has contributed to extremely high infection rates of a pathogen that can cause leprosy in Pará, Brazil.
An international team led by researchers at Colorado State University has found that human contact with wild armadillos — including eating the meat — has contributed to extremely high infection rates of a pathogen that can cause leprosy in Pará, Brazil.
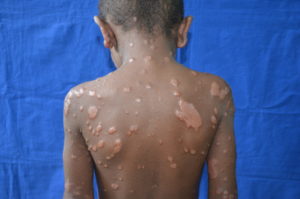
Mycobacterium leprae can cause leprosy, a chronic disease characterized by lesions of the skin and nerve damage, in humans. Other researchers have previously documented transmission of M. leprae to humans by nine-banded armadillos in the southern United States.
The findings from this new research have implications for public health education programs related to these mammals and zoonotic transmission, or the spread of infection between animals and people.
The study, “Evidence of zoonotic leprosy in Pará, Brazilian Amazon, and risks associated with human contact or consumption of armadillos,” was published in PLOS Neglected Tropical Diseases.
Armadillos have been shown to transmit M. leprae to people in Texas, Louisiana and Florida, where humans come into contact with the animals. But when Juliana Portela, a graduate student at the Federal University of Pará in Brazil, proposed conducting a survey of people who hunt, kill and eat armadillos to see if they were at increased risk for leprosy, her advisors — including CSU’s John Spencer — were skeptical.

“In the western Pará state in Brazil’s Amazon region, leprosy is already hyper-endemic,” said Spencer, senior author of the study and an associate professor in the Department of Microbiology, Immunology, and Pathology.
In Brazil, clinicians diagnose about 25,000 cases of leprosy each year. In comparison, the total number of new leprosy cases found in the U.S. is about 200 each year.
“This region [western Pará] has one of the highest new case detection rates in the whole country,” Spencer explained. “More than 50 percent of people in this area, on average, will be positive for the antibody, PGL-I, and the rate is even higher, over 90 percent, for some leprosy patients.”
A person can test positive for the antibody but still not have the disease, Spencer said. Testing positive for the antibody means that a person has been infected with M. leprae, but it is not a good indicator of disease progression. The best way to diagnose the disease is through clinical signs and symptoms, including skin lesions, loss of sensation and nerve damage, pain and inflammation.
Survey sought answers about contact with armadillos
The research team, which also included scientists from Switzerland and the Netherlands as well as three universities in Brazil, surveyed 146 people living in the town of Belterra. Scientists asked questions about the extent of contact with armadillos: Did they hunt or kill the animals, handle armadillo meat, or eat the meat?
What they found was astonishing, said Spencer:
- 65 percent of people surveyed had some contact with armadillos
- 65 percent were involved in either cleaning the meat or preparing it for cooking, and
- 65 percent also ate armadillo meat at least once a year.
More than 18 percent, or 27 people, identified themselves as hunters.
The researchers analyzed blood samples from people, as well as tissue samples from the liver and spleen of the animals killed by the hunters, for evidence of infection with M. leprae. People participating in the study also received a free exam by experienced leprosy clinicians, and those diagnosed with the disease received free treatment from a local health clinic.
Scientists found a positive antibody test in 63 percent of the people who took part in the survey. The team did not find much of a difference between people who ate or did not eat armadillo meat, and Spencer said there was not a major difference between people who cleaned the animals and prepared the meat or not, or in those who hunted or did not hunt the mammals.
Greater risk with more consumption
But the most startling finding was in people who ate armadillo meat frequently — more than once a month and, in some cases, twice a week. The strength of the antibody in these individuals was 50 percent higher than the other groups.
“Overall, they had a lot of risk factors, and a lot more exposure to armadillos than other people in the group,” said Spencer.
What the team found makes educating the public — in Brazil, the U.S. and around the world — extremely important, he added.
“You can get diseases from eating all kinds of food,” he said. “Millions of people eat sushi every day. Do people think about putting raw fish in their mouth?”
Similarly, with leprosy circulating from humans to animals (and the reverse), if you’re going to eat armadillo, take precautions. Spencer recommends wearing gloves when cleaning the carcass, and make sure to cook the meat until it is well-done.
“Your risk of picking up the disease from eating well-cooked meat is almost zero,” he said.
The research team is following up this study by sequencing the genome of this strain of M. leprae to learn more about what type of infection is circulating and how it might differ from strains found in the U.S. and elsewhere.
Co-authors of this study include scientists and clinicians from Colorado State University (Mary Jackson, John Belisle and Mercedes Gonzalez-Juarrero), École Polytechnique Fédérale de Lausanne in Switzerland (Stewart Cole and Charlotte Avanzi), Leiden University Medical Centre in the Netherlands (Annemiek Geluk), Federal University of Pará, Belém, in Brazil (Claudio Salgado, Josafá Barreto and Moises Batista da Silva), Universidade Federal do Oeste do Pará, Santarém in Brazil (Antonio Minervino) and the University of São Paulo Medical School in Ribeirão Preto, Brazil (Marco Andrey Cipriani Frade).